The reality of complications in epidural anesthesia needs to be confronted head-on. There’s room for improvement. We’ve seen plenty, as have many anesthesiologists — and patients. With Accuro ultrasound guidance for neuraxial anesthesia, anesthesiologists can see this reality and meet it with a new perspective.
By giving clinicians an accurate way to visualize and navigate intricate spinal anatomy, Accuro confronts the complexity and uncertainty behind common complications like dural punctures and nerve irritation. This technology has been proven to not only increase the success rate of first attempts but also reduce needle adjustments. The outcomes? Faster workflows, safer procedures, and significantly improved patient comfort.
The Accuro perspective: AI-enhanced visualization
Neuraxial ultrasound is primarily based on imaging of spinal bone structures. Accuro’s bone-to-tissue contrast — combined with AI-enabled landmark identification — provides anesthesiologists with unprecedented precision when placing neuraxial blocks:
- Automated identification and depth measurement: Accuro automates the identification of the epidural space, a crucial target for successful anesthesia delivery. It also measures the depth to this space, reducing guesswork and allowing for a more precise needle selection based on patient anatomy. This is especially helpful for patients with a high BMI.
- Enhanced bone structure visualization: Accuro’s ultrasound image reconstruction significantly enhances the contrast of bone structures. With higher bone contrast, the spinous process, articular process, and vertebral body become much clearer and more distinguishable on the screen. This bone-specific definition can tremendously improve the accuracy of landmark identification.
- Real-time pattern recognition for key landmarks: Accuro automatically recognizes key neuraxial landmarks using pattern recognition software. These landmarks include the spinous processes and interlaminar spaces. Having these structures automatically identified on screen streamlines workflows and empowers anesthesiologists to make informed decisions about needle placement.
Through this advanced visualization, Accuro becomes an invaluable assistant, giving anesthesiologists a new and enriched perspective when neuraxial blocks are placed.
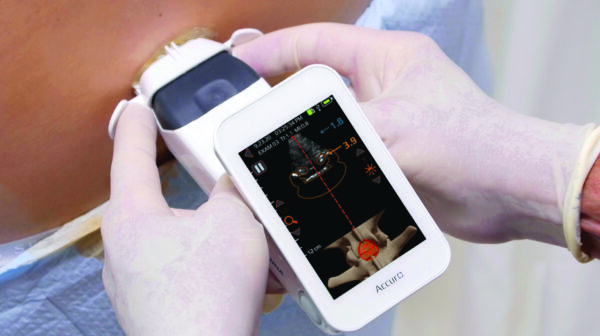
The results of enhanced visualization
Accuro’s guidance leads to a higher success rate on first-attempt needle placements compared to traditional techniques relying solely on palpation.
In a 2021 study comparing the use of Accuro to traditional palpation for neuraxial anesthesia placements, clinicians found a significant increase in first-attempt success rates (72.5% vs. 40.0%) when using Accuro compared to palpation. They also determined a decrease in the need for needle adjustments (40.0% vs. 72.5%) when placements were guided by Accuro. Overall, the study established that Accuro improved not only procedural efficacy and patient safety but also clinical training, noting:
“[Accuro] seeks to overcome many of the limitations of traditional ultrasound through a new ultrasound image reconstruction technique that significantly enhances bone structure contrast along with a new image postprocessing technology that automatically recognizes key neuraxial landmarks in real-time. Together, these novel technical features seek to flatten the learning curve by making bone landmark structures more readily apparent and providing automated image interpretation, which serves as a secondary confirmation of the anatomical features contained within the ultrasound image.”
These measured results spell faster procedures and less discomfort for patients. And they’re not outliers. In a 2023 study — also comparing traditional palpation-guided and ultrasound-guided needle placements — researchers found Accuro reduced complications associated with the epidural procedures. Imprecise needle placement can result in unintentional dural puncture. Accuro’s visualization of anatomical structures improves procedural precision, minimizing the risk of accidental needle insertion into the dura mater or nerves. This enhanced precision is evident in the study’s findings. While unintentional dural puncture with an epidural needle occurred in five patients in the group where palpation guided placements, none occurred in the group where ultrasound guided needle placement.

Accuro perspectives meet anesthesiologist perspectives
Accuro’s user-friendly interface and automated features also make it accessible to a wider range of practitioners. Unlike traditional ultrasound systems that require significant expertise in image interpretation, Accuro streamlines the process. The automated recognition of neuraxial structures eliminates the need for extensive ultrasound training, allowing even those with limited experience to perform epidural anesthesia with greater confidence. This is a boon for busy urban hospitals, low-resource rural providers, and underserved health centers alike.
Feedback from anesthesiologists who have adopted Accuro highlights its transformative impact on their practice. Many report Accuro’s visualization as instrumental in elevating procedural confidence and reducing complexities. Numerous practitioners have utilized its detailed imaging and automated precision to assist in procedural planning — particularly in difficult cases. These clinicians and anesthesiologists consistently report the same thing: better outcomes and fewer complications when using Accuro to administer neuraxial blocks.
Better visualization — better patient care
Acknowledging complications is the first step toward reducing them. Embracing Accuro isn’t about modernization or keeping up with new trends in medical technology. It’s about making a difference in workflows, patient experiences, and clinical outcomes. If the technology is available to make epidural anesthesia safer, faster, and more effective, we need to celebrate it. That’s our perspective. Will you help us share it?

