Medical Contributors

Adam Dixon, PhD
CTO, RIVANNA

Antonio Gonzalez-Fiol, MD
Assoc. Prof, Anes.; Dir, OBANES Fellowship, Yale

Stephen Garber, MD
Anesthesiologist, CA

Brian W. Launius, MD
Anesthesiologist, OH

Craig Loomis, MBA
Sr. Dir, Prod. Mgt., RIVANNA

Will Mauldin, PhD
CEO & Co-founder, RIVANNA

Paul Sheeran, PhD
Dir, R&D, RIVANNA

Christopher Thom, MD, RDMS
Assoc. Prof, EM, VA

Brandon M. Togioka, MD
Assoc. Prof & Vice Chair, Clin. Res., OHSU, OR
Medical Contributors

Adam Dixon, PhD
EVP, Eng., RIVANNA

Antonio Gonzalez-Fiol, MD
Assoc. Prof, Anes.; Dir, OBANES Fellowship, Yale

Stephen Garber, MD
Anesthesiologist, CA

Brian W. Launius, MD
Anesthesiologist, OH

Craig Loomis, MBA
Sr. Dir, Prod. Mgt., RIVANNA

Will Mauldin, PhD
CEO & Co-founder, RIVANNA

Paul Sheeran, PhD
Dir, R&D, RIVANNA

Christopher Thom, MD, RDMS
Assoc. Prof, EM, VA

Brandon M. Togioka, MD
Assoc. Prof & Vice Chair, Clin. Res., OHSU, OR
70 Birth Statistics and Facts
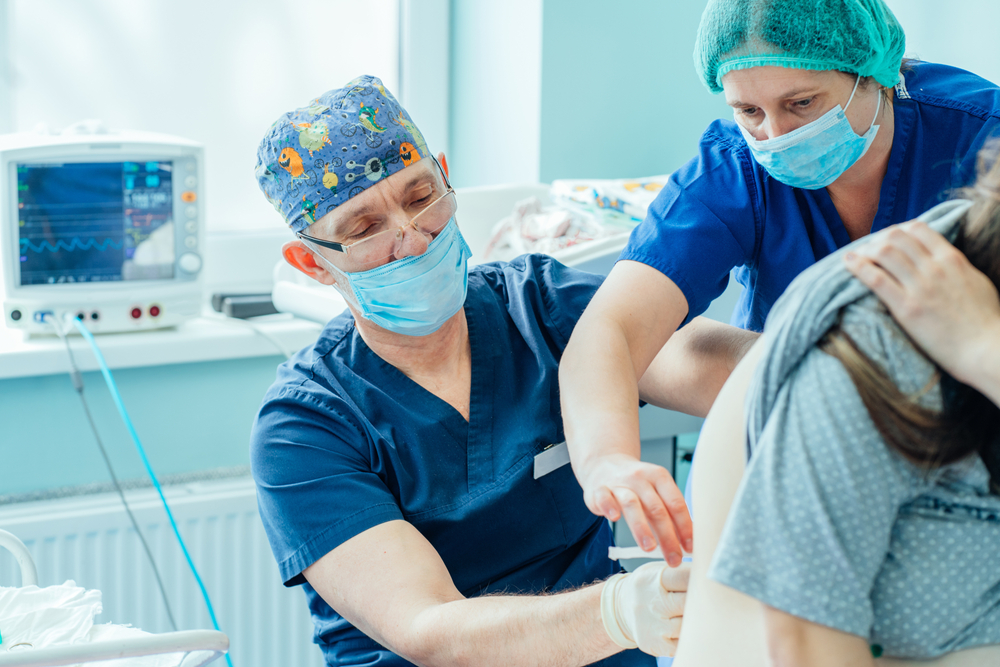
Whether you're a healthcare professional, expectant parent, or curious reader, these data points offer a snapshot of what childbirth looks like around the globe today. Dive in to see how birth is changing and how innovation is helping to make it safer for families...
32% Cesarean Rate Drives Demand for First-Attempt Neuraxial Success
The United States sees approximately 3.66 million births each year, with birth rates highest in states like Texas, California, and Florida. But behind these numbers, providers across the country are managing increasingly complex cases. More women are having...
Solving the Blind Procedure Problem in Modern Obstetric Anesthesia
In labor and delivery, every procedure brings unexpected variables — even for those who've spent their careers on the obstetrics floor. Unpredictability defines work in these units: a place where Dr. Hilary Gallin has spent years mastering anesthesiology's most...
RIVANNA’s 2025 Year in Review: Medical Imaging Innovation Across U.S. Healthcare
2025 was a defining year for RIVANNA as we connected with anesthesiology providers, healthcare innovators, and research leaders across the United States. From clinical symposia and pitch competitions to academic conferences and a moment in Times Square, our mission...
Global Neuraxial Practices: How Regional Differences Shape Patient Outcomes
Neuraxial anesthesia is not practiced uniformly across the globe. From the operating rooms of major academic medical centers to district hospitals in resource-limited settings, the techniques, protocols, and outcomes associated with spinal and epidural anesthesia...
RIVANNA announces FDA clearance of Accuro 3S Needle Guide Kit
CHARLOTTESVILLE, VA, DECEMBER 16, 2025 — RIVANNA®, developer of world-first imaging-based medical technologies, today announced that the U.S. Food and Drug Administration (FDA) has granted 510(k) clearance for its Accuro® 3S Needle Guide Kit consumables. This...
Advancing Obstetric Anesthesia: Dr. Steven Garber on the Real-World Power of Accuro 3S
Featuring Dr. Steven Garber, Obstetric Anesthesiologist, Saddleback Hospital In the delivery suite, precision is personal. Every placement, every decision, can shape a mother’s experience of birth. For Dr. Steven Garber, an obstetric anesthesiologist with more than...
Building Healthcare Equity in Modern Health Systems
Building health equity is an important role for modern health systems and hospitals. It’s an essential component of healthcare excellence in the areas of safety and quality. Medicine and healthcare still have a long way to go to make truly equitable care a reality,...
Up to 92% First-Attempt Success: How AI Quality Improvement Is Transforming Neuraxial Anesthesia
In neuraxial anesthesia, every decision is defined by precision. A single millimeter can shape patient comfort, safety, and outcomes. As artificial intelligence (AI) enters the perioperative space, it brings more than computational power; it brings clarity....
How 63% Fewer Readmissions Start with Smarter Healthcare Efficiency and AI
The healthcare environment in the US is one of constant change and fluidity. Changing demographic trends, economic forces, and advances in medical research and technology have significant impacts on healthcare and hospital performance and operations. The modern...
RIVANNA awarded $3 million CDMRP grant to develop military-optimized ultrasound guidance system for spinal interventions
CHARLOTTESVILLE, VA, OCTOBER 21, 2025 — RIVANNA®, developer of world-first imaging-based medical technologies, has recently been awarded with a Peer-Reviewed Medical Research Program (PRMRP) Technology/Therapeutic Development Award (TTDA) from the Congressionally...
10% Lower OR Costs: How Neuraxial Anesthesia Is Delivering Measurable Hospital Savings
Healthcare economics have never been more challenging. Rising costs, flat reimbursements, and pressure for quality outcomes mean every clinical decision has a financial impact. At the same time, payers are stripping away traditional payment modifiers, making it...
What is Neuraxial Anesthesia? A Data-Driven Look at a Key Pillar in Modern Healthcare
For hospital healthcare executives, navigating the complex landscape of clinical outcomes, patient satisfaction, and financial performance is a constant balancing act. Within this landscape, neuraxial anesthesia, which is a cornerstone of modern surgical and...
RIVANNA named a finalist in Medtech Innovator’s 2025 Early-Stage Grand Prize competition
CHARLOTTESVILLE, VA, OCTOBER 2, 2025 — RIVANNA®, developer of world-first imaging-based medical technologies, today announced it has been named a finalist in MedTech Innovator’s (MTI) 2025 Early-Stage Grand Prize competition. The recognition comes as part of the...
Accuro 3S-MIL: Collaborative Innovation for Military Healthcare Applications
Military medical device development requires more than adapting existing technology; it demands understanding operational realities from the ground up. The Accuro 3S-MIL development process exemplified this approach through a comprehensive 36-month timeline that...
Advancing Military Medicine With AI-Enhanced Ultrasound
By Paul Sheeran, Ph.D. — Director of Research & Development at RIVANNA For over a decade, RIVANNA has been at the forefront of imaging innovation, developing AI-driven procedural guidance to improve clinical outcomes. Now, with the support of a $3M...
AI is Revolutionizing Healthcare Quality: Tackling the 138,000 Nurse Shortage in 2025
The tech industry is continuing to advance their AI tools, such as large language models (LLMs) and beyond, in leaps and bounds. These tools are beginning to have major impacts in many areas, such as education, the workplace, and healthcare. The healthcare field is...
RIVANNA awarded $2.21 million NIH grant to develop pediatric lumbar puncture ultrasound guidance system
CHARLOTTESVILLE, VA, SEPTEMBER 2, 2025 — RIVANNA®, developer of world-first imaging-based medical technologies, has been awarded a $2.21 million Small Business Innovation Research (SBIR) Direct to Phase II (R44) grant from the National Cancer Institute (NCI) of the...
Accuro 3S-MIL: Purpose-Built Ultrasound Innovation for Military Spinal Procedures
Military healthcare providers face unique challenges when treating spinal conditions in deployed settings, where standard ultrasound equipment often falls short of operational needs. As a result, lower back pain significantly impacts military readiness, frequently...
Bridging Technology and Mission Readiness in Military Healthcare
Low back pain is one of the most common and costly challenges in military healthcare. It’s a leading cause of medical discharge, and it directly affects force readiness by delaying or preventing return to duty. For CRNAs, anesthesiologists, and pain management...
The Challenges of Bringing Neuraxial Ultrasound to Military Healthcare
Delivering the right solution often begins with understanding the right context. RIVANNA's introduction to the military healthcare sector was shaped not only by a product pitch, but by the realization that the primary challenge lay in mastering the language of the...
From Palpation to Precision: How Simulation Transforms Epidural Training Success Rates
The epidural procedure challenges even experienced anesthesiologists, yet we've trained generations using a system that leaves skill development largely to chance. Traditional training methods depend on whatever patients happen to walk through the door. Epidural...
RIVANNA secures $800,000 Virginia Catalyst Grant alongside matching funds to advance AI-enabled ultrasound platform for neuraxial anesthesia
CHARLOTTESVILLE, VA – AUGUST 14, 2025 — RIVANNA®, developer of world-first imaging-based medical technologies, was recently awarded grant funding valued at $800,000 from the Virginia Catalyst Program to advance the Accuro® 3S diagnostic ultrasound system. RIVANNA...
Where Do Handheld Devices Fit in the Modern Ultrasound Ecosystem?
Search interest for “handheld ultrasound” increased by 488% since 2010, reaching an average index of 43.4 in 2025. South Dakota and Kentucky are the states with the highest interest (100) in handheld ultrasound. Despite making up only 3.1% of the ultrasound...
Which State Should Be Most Concerned About Epidural Headaches?
How Obesity Shapes Public Concern and Complication Risks Across the U.S. States with higher obesity rates have much greater search interest in “epidural headache” (correlation r = 0.627, p < 0.001). West Virginia has the highest risk score at 93.5, indicating...
58% of Highly Engaged Hospital Staff Report Top Patient Safety Culture Scores
An analysis of the impact of employee engagement on hospital performance found 58% of the most engaged staff reporting top scores in patient safety culture. In the world of healthcare, patient safety by necessity plays a central role in ensuring quality healthcare;...
A 40% Obesity Rate Demands Precision Neuraxial Anesthesia
With obesity rates affecting over 40% of adults in North America, anesthesiologists are increasingly encountering situations where traditional palpation-based neuraxial techniques fall short. What was once considered a challenging subset of cases has become a...
BARDA awards nearly $10 million to RIVANNA to accelerate development of CADe/x AI module for Accuro XV
CHARLOTTESVILLE, VA – JULY 28, 2025 – RIVANNA®, developer of imaging-based medical technologies, announced that it received $9.92 million in federal funding of a contractual option from the Biomedical Advanced Research and Development Authority (BARDA), part of the...
RIVANNA’s next-generation ultrasound guidance platform and AI-driven imaging software receive FDA 510(K) clearance
CHARLOTTESVILLE, VA – JULY 15, 2025 – RIVANNA®, developer of world-first imaging-based medical technologies, announced that it has received 510(k) clearance from the U.S. Food and Drug Administration (FDA) regarding the Accuro® 3S diagnostic ultrasound system and...
Building a Health System to Support Aging Populations [6 Steps]
There is a significant shift occurring in the demographic composition of many developed countries: the aging of their populations. For the healthcare sector in the U.S., this presents a major challenge as a larger number of elderly people will need medical care....
Some Studies Show Up to 25% Fewer Assisted Deliveries With Low-Dose Epidurals
The management of labor pain has always walked a fine line between efficacy and impact on mobility. Traditional epidural techniques, while effective in pain relief, often result in significant motor block that limits maternal movement. This issue is increasingly at...
RIVANNA selected for prestigious MedTech Innovator 2025 Accelerator Cohort
— One of 65 startups chosen from nearly 1,500 global applicants — — Selected to participate in the world’s leading medtech accelerator — Charlottesville, VA, USA — June 9, 2025 — RIVANNA®, a medical device innovator and manufacturer focused on imaging-based medical...
Advancing Neuraxial Ultrasound With Dual-Array Probe Technology
In spinal anesthesia, precision isn’t optional — it’s foundational. Yet even with the increasing use of neuraxial ultrasound, traditional single-array probes still face key limitations: obstructed views, ambiguous needle trajectories, and inconsistent...
Neuraxial Ultrasound for Intuitive Spinal Imaging
For years, neuraxial ultrasound has promised to transform spinal access by offering real-time, image-guided precision. While its benefits are well documented, widespread adoption has been slowed by technical barriers and hesitation driven by usability limitations....
Advancing Military Healthcare Through Collaborative Innovation
Paul Sheeran, Ph.D. — Director of Research & Development at RIVANNA — explains how RIVANNA is working closely with military healthcare providers to drive medical innovation for military medical centers and military clinicians. Through strategic collaboration,...
A Snapshot of Healthcare in 2030
In 2025, the world of healthcare stands at a precipice. Myriad factors are converging that are poised to bring massive changes to the field. Disruptive, systematic shifts and major advances in technology and medical science could make the treatment centers,...
Patient-Centered Care With Ultrasound-Guided Epidural Placement
A high-risk labor case with prior anesthesia-related traumatic stress, extreme BMI, and comorbidities demonstrated how Accuro Neuraxial Guidance enabled safe, single-attempt epidural placement by providing real-time midline and depth confirmation. The handheld ultrasound system not only reduced procedural uncertainty but addressed the previous traumatic experience, improved patient trust, and allowed the anesthesiologist to deliver precise, effective analgesia where traditional techniques would likely have failed.
81% First-Pass Success: Why Neuraxial Anesthesia Needs Ultrasound Training Now
This content was reviewed by Stephen Garber, MD, Anesthesiologist in Southern California. Ultrasound has fundamentally changed how clinicians approach neuraxial anesthesia. For years, palpation has remained the primary technique for identifying neuraxial landmarks....
Reducing Variability in Neuraxial Access with AI and Procedural Design
How do you optimize one of the most technically challenging procedures in medicine? Paul Sheeran, Ph.D. — Director of R&D at RIVANNA — discusses a series of design interventions intended to reduce procedural variability in neuraxial ultrasound. Our approach...
Collaborative Innovation in Neuraxial Needle Guidance
Will Mauldin, Ph.D. — Chairman, CEO, and Co‑founder at RIVANNA — reflects on iterative paths to innovation in neuraxial ultrasound. Our ongoing collaboration with OB anesthesia providers and societies like SOAP has shaped the development of our continuous...
The Most Important Role for Healthcare Leadership
Healthcare executives have a lot of responsibility on their shoulders. Whether it’s making determinations about organizational structure or directing strategy, all top-down decisions can have significant consequences. However, perhaps the most impactful role that...
Preventing Post-Dural Puncture Headaches: Clinical Best Practices
This content was reviewed by Stephen Garber, MD, Anesthesiologist in Southern California. Post-dural puncture headaches (PDPH) are a widely recognized complication of spinal and epidural anesthesia, yet its prevalence remains a concern in modern anesthesiology....
Where is AI Working in Healthcare Today?
Artificial intelligence (AI) frequently makes headlines today. Many people are interested in keeping up with the latest advancements in large language models (LLMs) and other AI tools. However, AI has been playing a part in medical research for years, and today, it...
Breaking Barriers in Neuraxial Ultrasound Adoption
Reimbursement gaps and inconsistent complication reporting might be slowing the adoption of neuraxial ultrasound. Will Mauldin, Ph.D. — Chairman, CEO, and Co‑founder at RIVANNA — explains why these systemic challenges must be addressed to ensure advanced ultrasound...
Spinal Needle Guidance for Value-Based Care
Will Mauldin, Ph.D. — Chairman, CEO, and Co‑founder at RIVANNA — discusses the future of spinal needle guidance in a healthcare system still dominated by fee-for-service models. As the industry moves toward value-based care, RIVANNA is leading the way with...
The Future of Neuraxial Anesthesia
This content was reviewed by Stephen Garber, MD, Anesthesiologist in Southern California and updated in 2025 to reflect current clinical evidence and recent guidelines. Anesthesiology is in flux. Particularly in the United States, demographics, economics, and...
How Healthcare Executives Can Lead on Improving Healthcare Safety and Quality
In the field of healthcare and medical treatment, striving for improvements in healthcare safety and quality have always been of the utmost priority. As the medical field has evolved, great strides have been made in this area. Such advancements have contributed to...
Clinical Trials: Essential Parameters for Designing Studies
Chris Thom, MD, RDMS — Associate Professor of Emergency Medicine at the University of Virginia School of Medicine — discusses the key parameters for designing studies in clinical testing. ✅ : Ensuring patients fully understand the trial and provide legal...
AI-Assisted Neuraxial Anesthesia: Safety Meets Efficiency
The convergence of AI-guided neuraxial anesthesia and ultrasound-assisted anesthesia marks a profound shift in how we administer, teach, and measure the success of anesthesia procedures. With real-time data processing, image enhancement, and automated guidance, AI...
Benefits of AI-Driven Anatomical Guidance
Jaime Tierney Stanton — Ultrasound Systems Engineer at RIVANNA — discusses two key benefits of integrating AI-driven anatomical guidance and diagnostics into medical technology: Improved adaptability Improved efficiency 🔔 Follow us to stay up to date...
Advancement of AI Technology at RIVANNA
Will Mauldin, Ph.D. — Chairman, CEO, and Co‑founder at RIVANNA — has some thoughts about what’s on the horizon for AI-driven ultrasound innovation. As we innovate AI platforms for new clinical settings, real-world data is continuously fed back into AI training...
Validating Imaging-Based Medical Technology With Clinical Trials
Chris Thom, MD, RDMS — Associate Professor of Emergency Medicine at the University of Virginia School of Medicine — discusses the pivotal role of clinical trials in advancing medical care. Clinical trials, even at the feasibility stage, lay the groundwork for...
RIVANNA’s Long-Term Vision for Medical Imaging
Will Mauldin, Ph.D. — Chairman, CEO, and Co‑founder at RIVANNA — discusses a paradigm shift in how we innovate to create procedural efficiencies. While the journey to full clinical adoption takes time, RIVANNA is committed to advancing imaging-based solutions that...
Neuraxial Anesthesia: What is State of the Art in 2025?
Neuraxial anesthesia has long been a cornerstone of anesthetic practice, offering clinical benefits for a wide range of procedures, from labor and delivery to major surgeries. The field is constantly evolving, driven by technological innovation, updated guidelines,...
Leveraging the Latest Technology to Address Challenges in Healthcare Operations
Healthcare is an ever-evolving landscape that faces an array of challenges. As the United States and many other advanced economies experience an aging population, the demand for quality healthcare will continue to increase, placing additional strain on a system...
Elevating Care Through Meaningful Customer and Patient Engagement
Paul Sheeran — Director of Research & Development at RIVANNA — discusses our focus on enhancing both the patient experience and clinical outcomes by optimizing processes for providers, particularly recognizing the challenges many face with ultrasound technology. We...
Horizons for MedTech: Real-Time Needle Visualization in US-Guided Neuraxial Anesthesia
Will Mauldin, Ph.D. — Chairman, CEO, and Co‑founder at RIVANNA — emphasizes the need to overcome the long-standing challenges of real-time needle visualization in neuraxial anesthesia. Traditional ultrasound-guided procedures face two key barriers: 🚫 the...
Neuraxial Anesthesia Contraindications: An Evolving Conversation
Neuraxial anesthesia is a cornerstone of anesthetic practice, offering pain relief during surgeries, labor, and other medical procedures. However, there are specific contraindications — conditions or situations where neuraxial anesthesia poses unacceptable risks or...
RIVANNA examines regional trends in anesthesiology workforce and diagnostic imaging growth
CHARLOTTESVILLE, VA, DECEMBER 11, 2024 — RIVANNA®, developer of world-first imaging-based medical solutions, has released a report exploring trends in anesthesiology employment across the United States. The findings detail significant regional demand for...
Navigating Patient Acuity: Challenges in Obstetric Anesthesiology
Jacqueline Donovan, MD — Obstetric Anesthesiologist at Albany Medical Center — faces unique challenges every day, caring for patients with complex medical histories … or no medical history at all. She shares how Accuro is helping her practice improve patient...
Enhancing Obstetric Anesthesia: Perspectives from Dr. Matthew Sikora
Matthew Sikora, DO — Obstetric Anesthesiologist at MetroHealth Medical Center — emphasizes the importance of trusting your skills with neuraxial ultrasound. By confronting challenges with understanding, innovation, and technology, clinicians can: ✅ achieve...
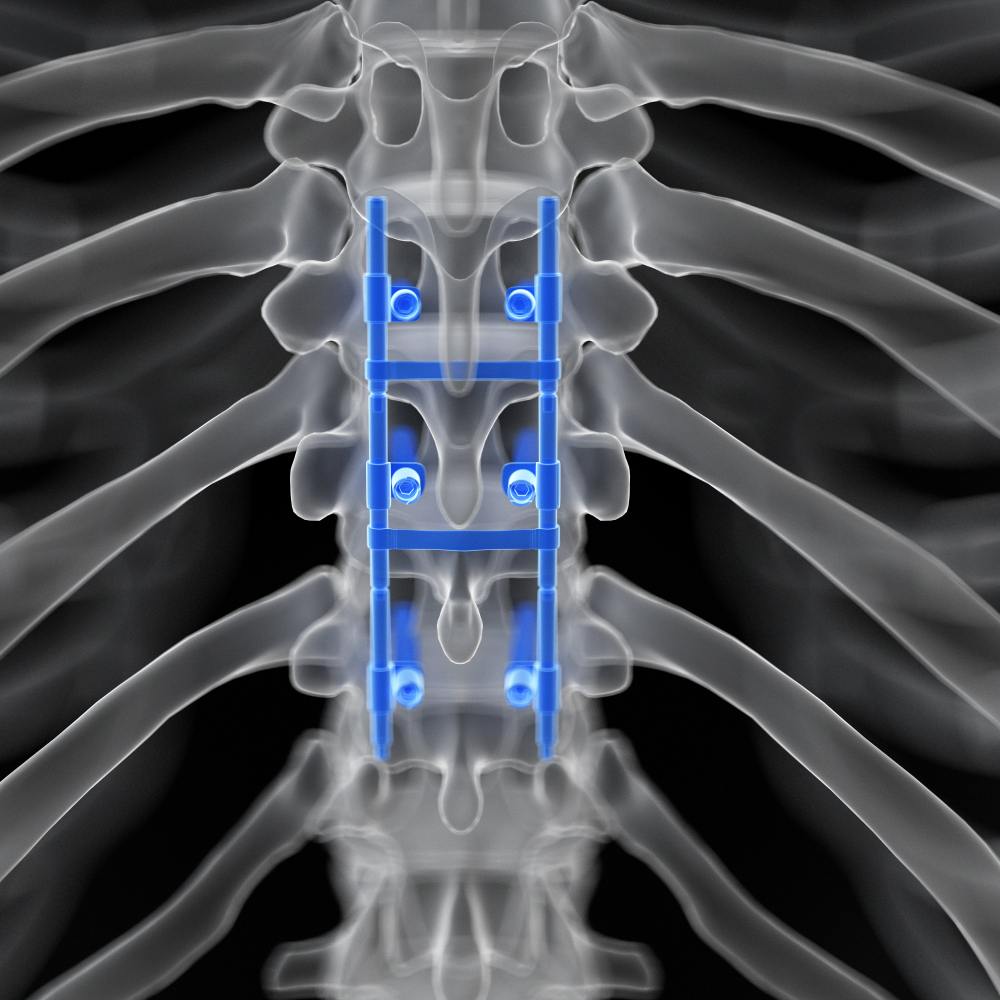
Neuraxial Anesthesia After Spine Surgery
Neuraxial anesthesia is a widely used technique for providing pain relief during surgeries and labor, but its application after spine surgery presents distinct challenges. Anatomical changes caused by surgeries such as laminectomies, spinal fusions, and disc...
Accuro 3S: Precision in Action
Neuraxial anesthesia is a critical procedure that can be challenging for clinicians and anxiety-inducing for some patients. The traditional reliance on blind palpation for needle placement presents significant challenges, particularly in complex procedures such as...
Breaking Ground With Accuro XV’s Feasibility Trial
Chris Thom, MD, RDMS — Associate Professor of Emergency Medicine at the University of Virginia School of Medicine — provides a detailed insider’s review of our Accuro XV feasibility trial. We’re investigating if ultrasound technology for musculoskeletal injury...
Ultrasound for Musculoskeletal Injuries: Accuro XV Feasibility Studies
Chris Thom, MD, RDMS — Associate Professor of Emergency Medicine at the University of Virginia School of Medicine — shares insights into the ongoing feasibility study for Accuro XV, a groundbreaking musculoskeletal ultrasound device. This feasibility study will...
6 Potential Complications of Neuraxial Anesthesia
Neuraxial anesthesia has become second nature to many practitioners, offering a reliable method for managing pain in surgery and labor. But even for seasoned anesthesiologists, the complications of neuraxial anesthesia remain a clinical reality that demands...
Neuraxial Ultrasound Guidance: Techniques, Methods, and Innovation
Ultrasound guidance is gaining traction for neuraxial procedures, providing anesthesiologists with enhanced accuracy, precision, and safety. Accuro — a handheld ultrasound guidance device for neuraxial procedures — was designed to integrate seamlessly into clinical...
Horizons for MedTech: Faster Diagnosis for Extremity Injuries
Chris Thom, MD, RDMS — Associate Professor of Emergency Medicine at the University of Virginia School of Medicine — breaks down how Accuro XV is set to simplify and speed up care for extremity injuries. Instead of the usual multistep process involving X-rays and...
Which U.S. States Have the Most Need for Anesthesiologists?
A new study by RIVANNA® analyzes employment trends in anesthesiology across U.S. states and the rapid growth of the ultrasound market, projected to double in value by 2034. We examine how technological advancements are transforming these medical fields, creating...
RIVANNA initiates multi-site first-in-human study for Accuro XV musculoskeletal imaging system
CHARLOTTESVILLE, VA, OCTOBER 8, 2024 — RIVANNA®, developer of imaging-based medical solutions, has announced the launch of the first multi-site study employing the Accuro® XV musculoskeletal imaging system. This milestone follows a $30.5 million funding option...
New Study: Growing Search for Anesthesiologist Jobs Across the U.S.
The role of the Anesthesiologist has been trending up over the last four years, and an increasing number of people want to know more about what this job entails. A new study by RIVANNA®, which aims to analyze the growth of search interest for anesthesiologist job...
New Study: Growing Interest in Certified Registered Nurse Anesthetists Across the U.S.
The role of the Certified Registered Nurse Anesthetist (CRNA) has recently gained significant attention. A new study by RIVANNA®, which aims to analyze the growth of search interest for “CRNA” across the United States, has revealed some significant findings. The...
RIVANNA secures patent for groundbreaking ultrasound-guided needle insertion system
CHARLOTTESVILLE, VA, SEPTEMBER 23, 2024 — RIVANNA®, developer of world-first imaging-based medical solutions, announced the acquisition of a groundbreaking patent for an advanced ultrasound-guided needle insertion system that promises to significantly enhance the...
Accuro’s Impact in CRNA Education
Beth Clayton — Professor and Program Director at the University of Cincinnati — shares her experiences using Accuro to enhance CRNA education. By simplifying the process of identifying midline and intervertebral spaces, Accuro reduces the need for multiple...
Meaningful Innovation: The Backbone of RIVANNA’s Story
We’re RIVANNA. We develop and commercialize comprehensive imaging solutions for spinal needle interventions and fracture and soft tissue diagnostics to improve provider precision and patient care. That’s what we do, and in many ways, it’s who we are. But here’s the...
Accuro Neuraxial Guidance: Current and Future Use Cases
Anesthesiologist Dr. Stephen Garber discusses special use cases for Accuro Neuraxial Guidance. Discover how this ultrasound-guidance device improves precision and patient safety, as well as how Dr. Garber sees this technology impacting anesthesiology in the future....
CRNAs Can Drive the Adoption of New Technologies for Patient Care
Certified Registered Nurse Anesthetists (CRNAs) are at the forefront of patient care, supporting safe, effective, and increasingly accessible anesthesia administration. As healthcare technology continues to evolve, CRNAs have the unique opportunity to lead the...
Ultrasound Guidance Is Changing Anesthesiologist Roles
A change is coming to acute pain management, and anesthesiologists are at the forefront. Ultrasound guidance has expanded the role of anesthesia providers by enhancing precision, safety, and efficiency in anesthesia administration. It enables more accurate needle...
Horizons for MedTech: AI, Ultrasound, and Next-Gen Neuraxial Guidance
Kathryn Ozgun — Sr. Ultrasound Systems Engineer at RIVANNA — has a sneak peek for those of you asking about our next generation of the Accuro product line. We’re wrapping R&D efforts on neuraxial guidance technology with some groundbreaking advancements in device...
Horizons for MedTech: Collaboration Toward Better Healthcare Solutions
Craig Loomis — Senior Director of Product Management at RIVANNA — explains our process for keeping partners informed, sharing feedback, and iterating together. Progress happens when conversations shift from “me” to “we.” At RIVANNA, this is always a critical...
How Accuro Supports CRNA Education
Nurse anesthesia education requires precision, hands-on practice, and the ability to navigate complex anatomical structures. Beth Clayton — seasoned Professor and Program Director at the University of Cincinnati — emphasizes the critical role of effective teaching...
Accuro’s Impact in Labor and Delivery
Anesthesiologist Dr. Stephen Garber describes Accuro’s ultrasound guidance for neuraxial anesthesia as an indispensable tool in his practice. Learn how this AI-powered device helps anesthesiologists personalize care, enhancing confidence and procedural precision...
Horizons for MedTech: Real-Time Needle Imaging for Neuraxial Anesthesia
Craig Loomis — Senior Director of Product Management at RIVANNA — gives an insider’s look at RIVANNA’s upcoming innovations in ultrasound guidance for neuraxial anesthesia. We’re developing cutting-edge solutions that address clinical challenges and improve medical...
RIVANNA: Collaboration Meets Innovation To Enhance Patient Care
Craig Loomis — Senior Director of Product Management at RIVANNA — shares his passion for improving healthcare through medical technology, especially through collaboration with clinicians. By addressing clinical challenges and connecting healthcare providers with...
Horizons for MedTech: Let’s Celebrate Patient-Centered Innovation
Antonio Gonzalez, M.D. — Associate Professor of Anesthesiology at Yale School of Medicine — highlights the importance of embracing technological innovations in healthcare for improved patient care. While technology might initially challenge our sense of control, it...
Precision in Medicine Is Compassion in Care
A patient waiting to receive spinal anesthesia for the first time is invariably anxious — and understandably so. At RIVANNA, every investment we make in research and development for our medical technology is guided by a commitment to helping clinicians improve that...
How Accuro Made Epidural Administration Possible for a Patient With Severe Scoliosis
Neuraxial anesthesia is a cornerstone in obstetrics for labor and delivery. Epidural placement requires exceptional precision, as any inaccuracies can lead to serious complications such as nerve damage or ineffective pain management. Dr. Stephen Garber, an...
How Ultrasound Guidance Mitigates Risks in Epidural and Spinal Anesthesia
In medicine, small errors can have profound implications. And in epidural and spinal anesthesia, sacrifices in precision correlate to sacrifices in patient care. It’s that simple. These procedures — absolutely crucial for pain management through childbirth and...
AI-Enhanced Ultrasound Guidance Improves Epidural Placement
Anesthesiologist Dr. Stephen Garber demonstrates how Accuro's AI-enhanced neuraxial ultrasound guidance improves epidural placement. This is a level of precision traditional methods can’t match. Discover how Accuro helps anesthesiologists pinpoint optimal depth and...
Accuro: Ultrasound-Enabled Perspective
The reality of complications in epidural anesthesia needs to be confronted head-on. There’s room for improvement. We’ve seen plenty, as have many anesthesiologists — and patients. With Accuro ultrasound guidance for neuraxial anesthesia, anesthesiologists can see...
Successful Placement of a Labor Epidural in a Patient With Severe Thoracolumbar Scoliosis With the Assistance of Image-guided Ultrasound
Background Conventional ultrasound has successfully displaced blind palpation for needle guidance procedures that include central venous access and peripheral nerve blockades. Additionally, the benefits of ultrasound guidance are increasingly clear for assessing and...
RIVANNA appoints Craig Loomis as senior director of product management
FOR IMMEDIATE RELEASE CHARLOTTESVILLE, VA, March 28, 2024 — RIVANNA®, a developer of imaging-based medical solutions, names Craig Loomis as senior director of product management. With over 25 years of extensive experience in global product development and...
Innovating Against Odds: Ultrasound Guidance for Complex Anesthetic Procedures
In anesthesiology, precision should never be a luxury. And in complex anesthesia, where the margin for error is razor-thin, absolute precision must be a baseline — it must be accessible, affordable, and effective. We’ve seen anesthesiologists navigate a minefield...
AI-Enhanced Ultrasound in Modern Anesthesiology
Anesthesiology is entering a dramatic renaissance. The traditional reliance on anatomical landmarks and intuition for neuraxial block placement is being rapidly replaced by earned confidence in artificial intelligence and ultrasound technology. This powerful...
Smarter Workflows Mean Better Outcomes: Workflow Intelligence for Ultrasound-Guided Neuraxial Anesthesia
Artificial intelligence (AI) is making ultrasound-guided neuraxial anesthesia easier for both novice and experienced healthcare providers to learn and adopt. Adam Dixon, Ph.D. — Vice President of Engineering at RIVANNA — explains how AI-enabled ultrasound guidance...
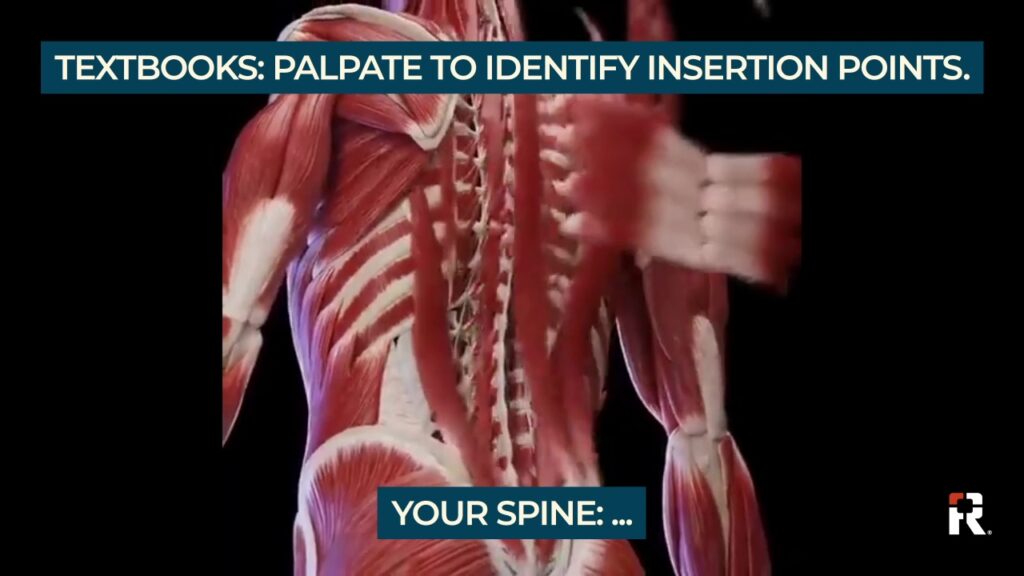
How Hard It Is To Palpate …
The complexity of spinal muscle systems — comprising multiple overlapping layers while varying widely in tone and bulk — significantly complicates palpation to identify insertion points for neuraxial anesthesia. Muscle dynamics and the presence of adipose and...
Accuro Improves Epidural Administration for Patients with Scoliosis
Epidural administration can be difficult for patients with anatomical complexities, particularly scoliosis. The procedure encompasses placing neuraxial blocks for surgical treatments and child delivery, and it demands precision that traditional methods — reliant...
How the Closure of Rural Hospitals Affects Anesthesiology
In the quiet expanses of rural communities, the lights of hospitals are going out as facilities close. It’s a silent crisis that starkly affects both patients and medical professionals, with a serious impact on anesthesiology. As rural hospitals shut their doors,...
How It’s Different From Traditional Ultrasound
Accuro is improving patient care and administrative efficiency in low-resource settings. Anesthesiologist Dr. Audrey Alleyne discusses the tremendous benefits of the Accuro Neuraxial Guidance device for spinal and epidural anesthesia where time and access to...
Accuro in Difficult Epidurals
Dr. Yunus Shah, attending anesthesiologist, describes the convenience and efficiency of using the Accuro Neuraxial Guidance device for anesthesia to accomplish epidural placement in challenging Advanced epidural guidance means improved outcomes for clinicians...
Dr. McMullan: A Tool To Increase Success Rates and Decrease Placement Time Is Genius
Patients with complex anatomies – such as those with an increased BMI or scoliosis – suffer more failed attempts at needle placement than other patients. That hurts the patient, frustrates the clinician, and wastes time. That’s why RIVANNA created the handheld...
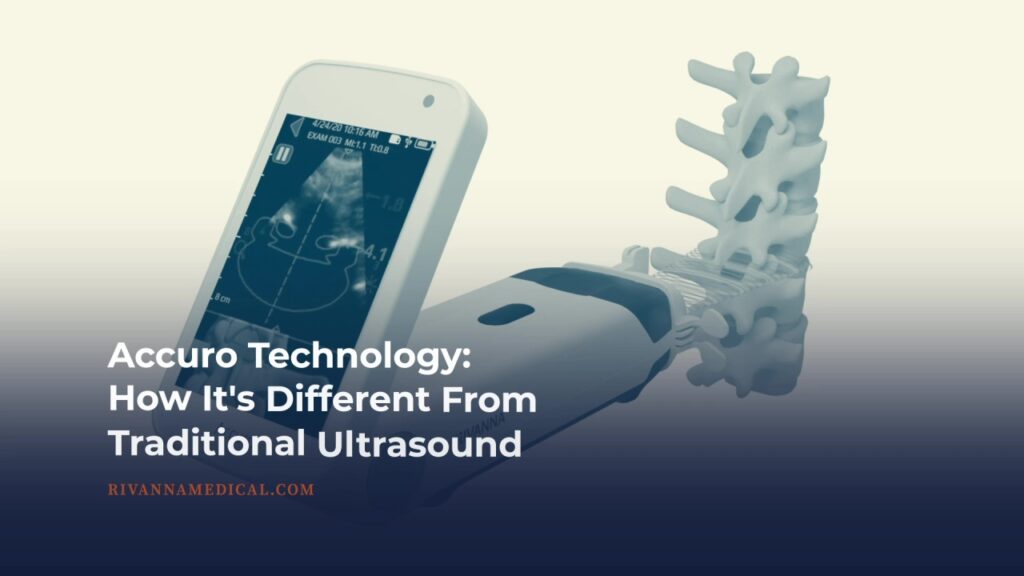
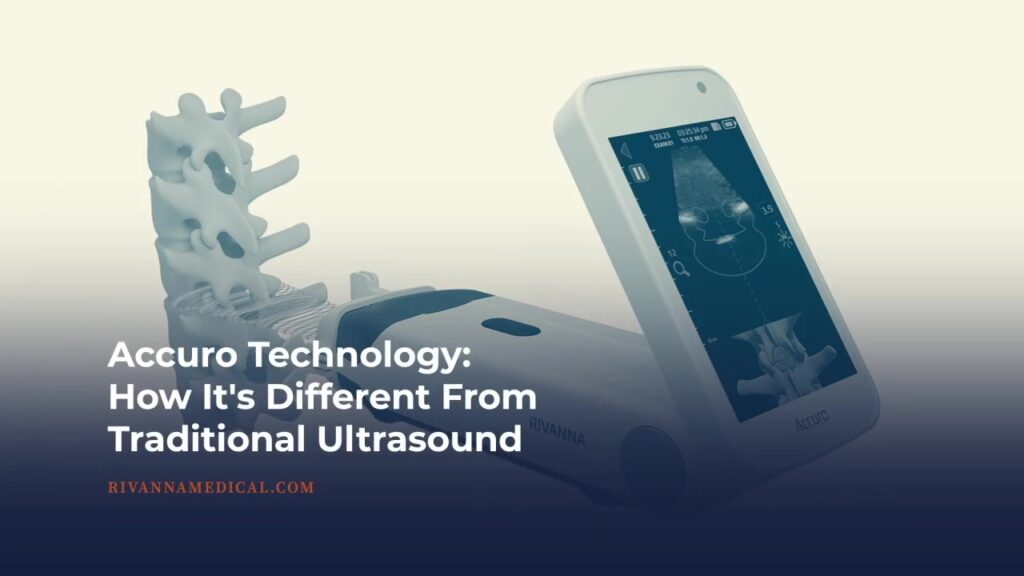
Accuro Technology: How It’s Different From Traditional Ultrasound
Dr. Will Mauldin, RIVANNA CEO and Co-Founder, saw a need in anesthesia for automated, real-time image guidance for epidurals. That prompted the development of the FDA-approved Accuro Neuraxial Guidance device, an ultrasound-based imaging solution for epidural and...
The Challenges of Traditional Ultrasound
Traditional ultrasound is a cornerstone in diagnostic and procedural medicine. But its application comes with a unique set of challenges, particularly in neuraxial procedures, where precision is nonnegotiable. From the steep learning curves associated with image...
Mitigating Anesthesiology’s Biggest Stressors: How Accuro Neuraxial Guidance Technology Can Help
These days, just about any job carries what feels like an incredible level of stress. But few careers actually match the stress of what it means to be an anesthesiologist or a certified registered nurse anesthetist (CRNA). This profession consistently ranks among...
How to Use Accuro – A Quick and Easy, Step-by-step Training Video
Dr. Antonio Gonzalez of the Yale School of Medicine demonstrates RIVANNA’S Accuro from start to finish, showing how neuraxial navigation is faster and more accurate with Accuro’s image guidance technologies that improve bone visualization and spinal landmark...
How Your Peers Are Reducing Complications by Over 80% With Accuro
Hear anesthesia providers describe their real-world experiences using RIVANNA’S Accuro Neuraxial Guidance technology for epidurals and spinals. See what your peers are doing to reduce complications by over 80% by addressing their challenges. Accuro Neuraxial...
An Accuro Success Story: Rapid Placement of a Neuraxial Block in a Morbidly Obese Parturient
The physiology of morbidly obese patients presents unique challenges when it comes to adapting medical procedures — including those that require anesthetization. Achieving successful neuraxial anesthesia can be particularly daunting due to impalpable landmarks and...
Challenges Facing Today’s CRNA (Accuro Can Help)
Certified registered nurse anesthetists (CRNAs) play a critical role in providing excellence in patient care. There’s an ever-growing need for the skills and experience that accompany this position, but extreme staffing shortages persist across the country....
CRNA Sweepstakes Winner Candid Feedback on Using Accuro
CRNA Kelli Camp describes how Accuro is “an amazing tool” that enables her small hospital to provide faster relief with greater confidence and give every patient a more effective epidural regardless of their size or body shape. Visit booth 525 at AANA or sign...
What Are the Benefits of Using Accuro?
What are the benefits of using Accuro? Dr. Beth Clayton, nurse anesthesia program director at the University of Cincinnati, explains how Accuro facilitates a more effective epidural, lowers complication rates, and optimizes the patient experience. We invite you to...
RIVANNA’s Growth Points to Innovative Partnerships
Will Mauldin, CEO and Co-Founder of RIVANNA, discusses his company’s mission to elevate the standard of patient care and the ways their ongoing partnership with BARDA, an agency within the Department of Health and Human Services, provides a unique opportunity to...
RIVANNA receives $30.5 million from BARDA to advance the Accuro XV musculoskeletal imaging system
CHARLOTTESVILLE, VA, JULY 26, 2023 — RIVANNA®, developer of imaging-based medical solutions, announced that they have received funding totaling $30.5 million over 39 months from early execution of an option by the Biomedical Advanced Research and Development...
The Use of Ultrasound in Neuraxial Anesthesia
Brendan Carvalho, MD, Chief of Obstetric Anesthesia, Stanford University Medical Center, shares his expertise about the widely accepted use and accuracy of ultrasound devices in neuraxial anesthesia, and his thoughts on the comparable Accuro device, which has the...
The Changing Face of Neuraxial Anesthesia – Speed, Safety, and Efficiency
Among the countless advancements in the field of medicine, neuraxial anesthesia stands out as a cornerstone of modern perioperative care. This specialized technique — involving the administration of local anesthetic agents near the spinal cord — has garnered broad...
Patient Success Story Using Accuro
Brandon Togioka, M.D., Associate Professor at Oregon Health & Science University and Vice Chair of Clinical Research for Anesthesiology @ OHSU, explains how Accuro enabled him to successfully administer a neuraxial epidural to a patient with scoliosis. To...
The Accuro Advantage: Better Epidural Placement in Patients with Musculoskeletal Disorders
Brandon Togioka, M.D., Associate Professor at Oregon Health & Science University and Vice Chair of Clinical Research for Anesthesiology @ OHSU, shares the benefits of Accuro for patients with complex anatomies. To learn more about how Accuro neuraxial...
Precision in Neuraxial Anesthesia: The Power of Clinically Proven Innovation
Neuraxial anesthesia is a vital component of anesthesiology, providing regional anesthesia for diverse surgical procedures. Anesthesiologists recognize its pivotal role in relieving pain and discomfort; however, it presents administration challenges when utilized...
Accuro epidural guidance device demonstrated superior for spinal anesthesia administration compared to palpation and conventional ultrasound in a parturient with extreme obesity
Accuro's integration of artificial intelligence with ultrasound (AI-US) provides detailed ultrasound image-analysis pivotal in complex clinical scenarios. CHARLOTTESVILLE, VA, August 16, 2022 — RIVANNA®, developer of world-first, imaging-based medical solutions,...
RIVANNA appoints medical technology veteran Nikki Troiano Gainey to board of directors
Medical Technology Leader to Advise Commercialization Strategy for Next-Generation Products CHARLOTTESVILLE, VA, July 7, 2022 — RIVANNA®, developer of world-first, imaging-based medical solutions, has named Nikki Troiano Gainey, a MedTech corporate and...
RIVANNA names Mikel Lewis director of manufacturing operations
Experienced Manufacturing Leader Integrates LEAN Principles to Maximize Quality and Productivity CHARLOTTESVILLE, VA, July 13, 2022 — RIVANNA®, developer of world-first, imaging-based medical solutions, has appointed Mikel Lewis, an experienced life science...
RIVANNA expands world-class engineering team to advance development of the Accuro product platform
CHARLOTTESVILLE, Virginia — RIVANNA®, developers of world-first, imaging-based medical solutions, today announced the appointment of Paul Sheeran, PhD, as senior ultrasound engineer to advance the development of RIVANNA’s next-generation product platforms,...
RIVANNA 2021 year in review
2021 continues to be an incredible year for us at RIVANNA—and we couldn't have done it without you. Thank you for being part of our journey to elevate the global standard of care. Best wishes for peace and prosperity in 2022; let’s make it extraordinary....
RIVANNA announces partnership with BOMImed to increase distribution of Accuro in Canada
CHARLOTTESVILLE, VA, DECEMBER 1, 2021 — RIVANNA®, developer of world-first, imaging-based medical solutions, announced they have entered into a partnership with BOMImed, a recognized manufacturer of anesthesia and critical care related consumables to represent and...
RIVANNA purchases new facility signaling rapid growth
CHARLOTTESVILLE, Virginia — RIVANNA®, developer of world-first, imaging-based medical solutions, today announced the purchase of a 10,000 square-foot facility in Charlottesville, Virginia, with acreage earmarked for new construction. The venture accommodates...
Accuro | Data Storage
Danielle Faulk answers some of the most frequently asked questions about Accuro. Accuro has maximum storage capacities of 10,000 images, 300 videos, and 999 exams....
RIVANNA announces award from U.S. government to develop Accuro Platform for rapid triage of blast-related injuries
CHARLOTTESVILLE, VA, OCTOBER 26, 2021 — RIVANNA®, developer of imaging-based medical solutions, announced that they have received a contract from the Biomedical Advanced Research and Development Authority (BARDA), a division of the Office of the Assistant Secretary...
RIVANNA’s Accuro shows statistically significant efficacy and safety for combined spinal-epidural anesthesia
CHARLOTTESVILLE, VA, SEPTEMBER 13, 2021 — RIVANNA®, developer of world-first, imaging-based medical solutions, today announced the results of a recent randomized controlled trial (RCT) showing that Accuro® automated spinal navigation system significantly enhanced...
RIVANNA’s Accuro automatically identifies and measures epidural space depth with accuracy equivalent to standard ultrasound in obese pregnant women
CHARLOTTESVILLE, VA, September 8, 2021 — RIVANNA®, developer of world-first, imaging-based medical solutions, today announced the results of a prospective, double-blind study demonstrating that the Accuro® Epidural Guidance device with SpineNav3D™ technology...
Dr. Garber Q&A
Q. As a practicing Obstetric Anesthesiologist, why did you decide to try Accuro for epidurals and spinals? A: I'm always pursuing new technology. I happened upon the Accuro booth at the SOAP meeting, was very intrigued, and decided to give it a try. As an...
Dr. Launius Q&A
Q. As a practicing Obstetric Anesthesiologist, why did you decide to try Accuro for epidurals and spinals? A: I first became aware of Accuro about four years ago. Practicing anesthesiology in a community-hospital setting for 25 years, I was always interested in how...
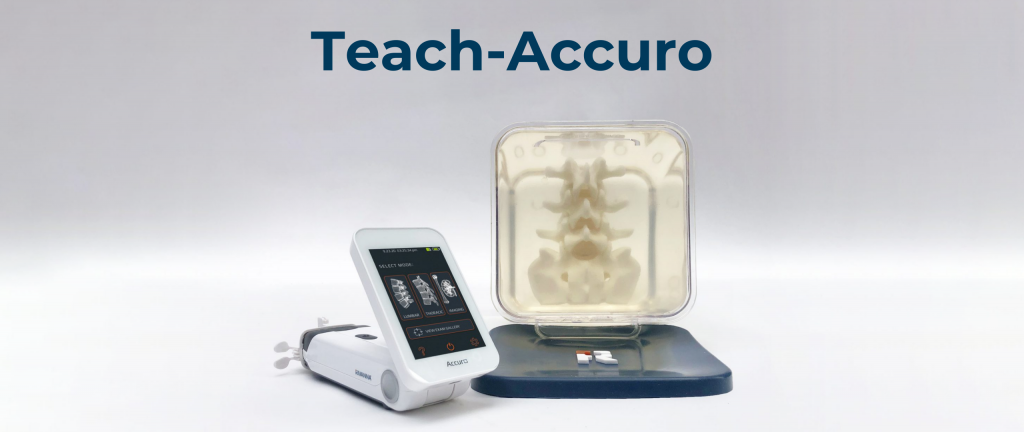
RIVANNA launches Teach-Accuro, a CRNA Educators Project
CHARLOTTESVILLE, VA, August 4, 2021 — RIVANNA®, developer of world-first, imaging-based medical solutions, today announced the first semester of the Teach-Accuro CRNA Educators Project. The new initiative provides the Accuro® spinal navigation system at no cost to...
RIVANNA announces record second-quarter Accuro sales
CHARLOTTESVILLE, VA, July 13, 2021 — RIVANNA®, developer of world-first, imaging-based medical solutions, today announced sales of the Accuro device and related service and equipment increased 263% versus the same period of the prior year following second-quarter...
RIVANNA’s Accuro product-line expansion fortified with European notice of allowance
CHARLOTTESVILLE, VA, JUNE 2, 2021—RIVANNA®, developer of world-first, imaging-based medical solutions, announced the European Patent Office has issued RIVANNA a notice of allowance for European patent application No. 13803513.4 entitled “Ultrasound Imaging of...
RIVANNA announces alliance with Tri-anim Health Services to increase nationwide distribution of Accuro
CHARLOTTESVILLE, VA, MAY 4, 2021—RIVANNA®, developer of world-first, imaging-based medical solutions, announced they have entered into a partnership with Tri-anim Health Services, a specialty distributor of respiratory, anesthesia, and critical-care supplies, to...
RIVANNA Announces Alliance with Tri-anim Health Services
CHARLOTTESVILLE, VA, MAY 4, 2021—RIVANNA®, developers of world-first, imaging-based medical solutions, announced they have entered into a partnership with Tri-anim Health Services, a specialty distributor of respiratory, anesthesia, and critical-care supplies, to...
United Kingdom’s NICE publishes Medtech innovation briefing on the use of Accuro
UK's NICE Publishes Medtech Innovation Briefing on Accuro for Guiding Epidural or Spinal Anaesthesia to Reduce Needle Insertions Compared with Palpation Alone in People with Obesity CHARLOTTESVILLE, VA., April 13, 2021—RIVANNA®, developer of world-first,...
RIVANNA launches Accuro Second Generation with Multi-Frequency Image Reconstruction and AI-Based Spine Recognition
RIVANNA Launches Accuro Second Generation With BoneEnhance® Multi-Frequency Image Reconstruction And SpineNav3D™ AI-Based Spine Recognition CHARLOTTESVILLE, VA., March 23, 2021 — RIVANNA®, developer of world-first, imaging-based medical solutions, announces...
RIVANNA launches second generation Accuro with thoracic functionality and globally enhanced performance
Real-time needle guidance for paramedian epidural and spinal anesthesia maximizes image guidance efficiency CHARLOTTESVILLE, VA., November 16, 2020 – RIVANNA® today announced launch of its second-generation Accuro® automated spinal navigation system, combining...
Intervertebral Level Identification and Image-guided Epidural Placement in Parturient Presenting Post-trauma Spinal Instrumentation and Scarring
Background Conventional ultrasound has successfully displaced blind palpation for needle guidance procedures that include central venous access and peripheral nerve blockades. Additionally, the benefits of ultrasound guidance are increasingly clear for assessing...
RIVANNA issued new patents for core Accuro technology
Growing Patent Portfolio Paves the Way for Product Line Expansion CHARLOTTESVILLE, VA., June 26, 2020 — RIVANNA® today announced three new patents for its Accuro® ultrasound-based spinal navigation system, bringing the company's portfolio covering its core...
RIVANNA to commercialize low-cost, bedside system to minimize non-diagnostic BMTB acquisition
Palpation alone to determine the appropriate needle trajectory is recognized as a contributing factor in the acquisition of non-diagnostic BMTB specimens [1, 2]. CHARLOTTESVILLE, VA, May 20, 2020 — RIVANNA announced that the company was awarded a $1.5M...
Neuraxial Guidance Device Beats Palpation-Guided Spinal Anesthesia in Obese Patients
Hand-held Ultrasound Device Accurate for Neuraxial Depth and Landmark Assessment
Adoption of Accuro automated spinal navigation system soars
Increasingly Practice Guidelines Recommend Image Guidance for Spinal Needle Placement Procedures CHARLOTTESVILLE, VA., February 19, 2020 — RIVANNA® today announced that sales of its Accuro ultrasound-based spinal navigation system more than doubled in 2019 compared...
Automated spinal navigation device reduced needle redirects by 48%
Latest Clinical Trial Results Highlight the Benefits of RIVANNA® Accuro® for Spinal Anesthesia in Patients Undergoing Orthopedic Surgery Automated Spinal Navigation Device Reduced Needle Redirects by 48% for Experienced Anesthesia Providers CHARLOTTESVILLE, VA.,...
RIVANNA Receives $800,000 Grant
Governor Northam Announces Life Science, Cancer Research Advancing in Virginia with $3.3 Million ‘Catalyst’ Awards: RIVANNA receives an $800,000 grant to develop Accuro 3S
OB/GYN Ultrasound
OB/GYN ultrasound: is the field ready to adopt new technology in the market?
Accuro Shows Improvements vs Blind Needle Guidance in RCT
RCT of 150 spinal anesthesia procedures demonstrates Accuro’s improved success rates, patient satisfaction, and needle insertion time versus blind needle guidance
An Accuro Success Story: Rapid Placement of Neuraxial Block in Morbidly Obese Parturient to Avoid General Anesthesia
Neuraxial ultrasound is proven to increase spinal and epidural success; however, a steep learning curve has prevented widespread adoption of this technology. Accuro’s SpineNav3D™ technology eases the training burden by automating identification of spinal...
Automated Ultrasound Guidance Streamlines Epidural Placement for Challenging Patients in Labor
It’s no secret that childbirth hurts. For most women, it is characterized by intense pain and pressure in the lower abdomen and back – and for some, this can be overwhelming. Many patients choose relief through epidural analgesia, which involves injection of a...
Ultrasound Streamlines Epidural Placement for Patients in Labor
Automated ultrasound guidance streamlines epidural placement for challenging patients in labor
Ultrasound guidance improves neuraxial anesthesia safety
Ultrasound guidance improves neuraxial anesthesia safety
RIVANNA tackles epidural failure rates with its hand-held imaging device
Rivanna tackles epidural failure rates with its hand-held imaging device
Wireless, handheld spinal ultrasound takes the guesswork out of epidural needle placement
Wireless, handheld spinal ultrasound takes the guesswork out of epidural needle placement
Local company develops ultrasound technology to facilitate anesthesia delivery
Local company develops ultrasound technology to facilitate anesthesia delivery
NIH: Pocket-sized imaging device improves accuracy of epidural placement
NIH: Pocket-sized imaging device improves accuracy of epidural placement
Hand-held Ultrasound Device Accurate for Neuraxial Depth and Landmark Assessment
Hand-held Ultrasound Device Accurate for Neuraxial Depth and Landmark Assessment
SOAP Clinical Research Presentations Prove the Benefits of RIVANNA Spinal Navigation System
SOAP Clinical Research Presentations Prove the Benefits of RIVANNA Spinal Navigation System
RIVANNA receives Health Canada approval for Accuro spinal navigation system
Rivanna Medical Receives Health Canada Approval for Accuro™ Spinal Navigation System
Accuro used in world’s first image-guided epidural in patient with rare neurological condition
Accuro™ used in world’s first image-guided epidural in patient with rare neurological condition
RIVANNA announces multiple key patents for Accuro and Accuro Locator
RIVANNA Announces Multiple Key Patents for Accuro™ and Accuro Locator™
RIVANNA secures $3.5 million in growth financing
RIVANNA Secures $3.5 Million in Growth Financing
RIVANNA awarded $1.5M NIH grant for rapid ultrasound-based 3D bone fracture assessment in the emergency department
RIVANNA Awarded $1.5M NIH Grant for Rapid Ultrasound-based 3D Bone Fracture Assessment in the Emergency Department
RIVANNA announces partnership with UK-based Vertec Scientific
RIVANNA Announces Partnership with UK-based Vertec Scientific
RIVANNA prepares for European market adoption of Accuro with the appointment of a new Vice President of Sales, Europe, the Middle East, and Africa (EMEA)
RIVANNA prepares for European Market adoption of Accuro™ with the appointment of a new Vice President of Sales, Europe, the Middle East, and Africa (EMEA)
RIVANNA launches international expansion in the Middle East with easy-to-use, automated ultrasound
RIVANNA Launches International Expansion in the Middle East with Easy-to-use, Automated Ultrasound
Accuro Highlighted in “AORA 2015” scientific presentation by Anand M. Sardesai, MD, anesthesiologist, Cambridge (UK) University Hospital: “Advances in Ultrasound Machine Technology and Future Trends”
Accuro™ highlighted in “AORA 2015” scientific presentation by Anand M. Sardesai, MD, Anesthesiologist, Cambridge (UK) University Hospital: “Advances in Ultrasound Machine Technology and Future Trends”
RIVANNA commences manufacturing of its Accuro device for launch at annual meeting of the American Society of Anesthesiologists (ASA)
RIVANNA commences manufacturing of its Accuro™ device for launch at annual meeting of the American Society of Anesthesiologists (ASA)
RIVANNA appoints Rebecca D. Minehart, M.D., Assistant Professor of Anesthesia, Massachusetts General Hospital, as a clinical advisor
RIVANNA appoints Rebecca D. Minehart, M.D., Assistant Professor of Anesthesia, Massachusetts General Hospital, as a clinical advisor
RIVANNA appoints Brendan Carvalho, M.D., Stanford Univ. Medical Center, as a clinical advisor
RIVANNA appoints Brendan Carvalho, M.D., Stanford Univ. Medical Center, as a clinical advisor
RIVANNA has received FDA clearance for Accuro
RIVANNA has received FDA clearance for Accuro™
Article features the RIVANNA UVA alumni
Article features the RIVANNA UVA alumni



















![Building a Health System to Support Aging Populations [6 Steps]](https://rivannamedical.com/wp-content/uploads/2025/06/Building-a-Health-System-to-Support-Aging-Populations-6-Steps.jpg)